Endometriosis Blog
- All Blogs
- Endo events
- Endo fundraising
- Endo medical
- Endo news and media
- Endo podcast
- Endo research and education
- Endo stories
- Endo support
- Fertility and pregnancy
- Mental health and wellbeing
- Relationships and sex
- EndoThrive
Priority Populations in Endometriosis
Priority Populations in Endometriosis: Global and Cultural Perspectives Endometriosis affects an estimated 1 in 7 women...
Endometriosis and Pelvic Pain Clinics in Australia
Endometriosis and Pelvic Pain Clinics in Australia: Putting Patients First People living with endometriosis and persistent...
Gender-Affirming Endometriosis Care
Gender-Affirming Endometriosis Care: Insights with Dr. Maddalena Giacomozzi Endometriosis is often described as a “women’s...
Endometriosis Out‑of‑Pocket Costs and Barriers to Care
$870 in Six Weeks: The Hidden Cost of Endometriosis and Pelvic Pain Last week, journalist Ima Caldwell published her...
Transgender Awareness Week: Max Jahufer
Transgender Awareness Week: Max Jahufer on Endometriosis and Pelvic Pain Transgender Awareness Week is a time to amplify...
New Endometriosis Clinics in Australia
Locations for 11 new Endometriosis and Pelvic Pain Clinics announced The Federal Government has announced the locations of...
Age and Endometriosis with Dr Lydia Coxon
Age and Endometriosis: Understanding Flares Across the Lifespan Endometriosis is a chronic condition that affects millions...
Endometriosis Australia’s statement on Victorian Women’s Pain Inquiry
Women’s Pain Inquiry: A Turning Point for Endometriosis and Female Health Endometriosis Australia welcomes the findings of...
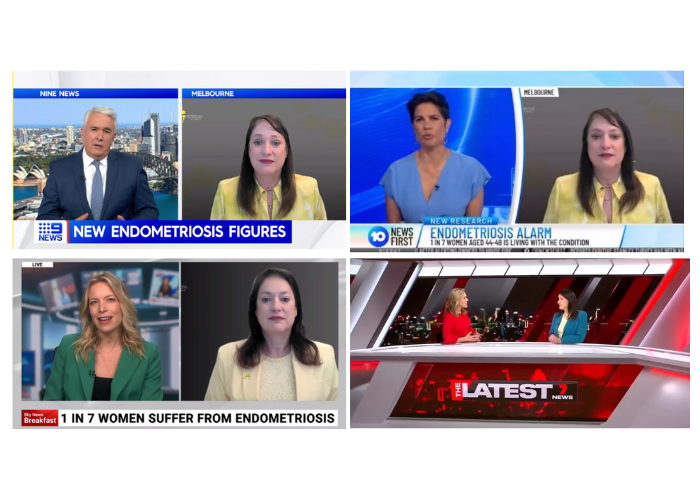
Study finds significant increase in endometriosis diagnoses and GP Referrals
Study Reveals Significant Increase in Endometriosis Diagnoses in Australian Women A new study has found the number of...
Endometriosis Behind the Pain Panel
Endometriosis Australia’s Chair, Monica Forlano, joined a panel of leading gynaecologists, women’s health specialists,...
International Women’s Day 2024
A call to action for employers who care about women's health and wellbeing International Women’s Day 2024 theme is...
Kayla Itsines Joins Forces With Endometriosis Australia as New Ambassador
Kayla Itsines was announced as Endometriosis Australia’s newest ambassador, at the FITHER Expo, Australia’s largest...
From leaps to bounds: Workplace Accreditation Program, Research updates, and more!
I am pleased to bring you some exciting updates. Straight off the bat, I congratulate the Australian Women’s Cricket...
Brisbane High Tea
Endometriosis Australia’s Brisbane High Tea was fabulous, with keynote speakers Premier Annastacia Palaszczuk and...
Singing the menstrual blues
Written by Kathy Lette Periods have always been a shameful secret. Tampon and panty liner ads are euphemistic, coy and...
Talking endometriosis: An expert panel
“Surgery is sexy. But you need a specialist that considers all complementary services. Surgery may be helpful, but it...
Endometriosis Australia’s Research Grant winners
Three researchers at the Royal Women’s Hospital will share in grants worth $30,000 from Endometriosis Australia....
EndoWarriors at Parliament
In our community, 1 in 10 women will have endometriosis. This is a startling figure that shows the level of impact on...
Luminosity 2017
Luminosity is a vibrant, fun 2 hour yogathon to raise awareness and funds into research of Endometriosis, a condition...
Kelsey Bright’s UK walk for endometriosis awareness
Kelsey Bright Takes on 1,600km Walk from Scotland to England to Raise $50,000 for Endometriosis Australia South...
7 creative ways to raise money for Endometriosis Australia through community fundraising.
Endometriosis is a condition that affects 1 in 7 women, yet its impact is often overlooked. At Endometriosis...
Introducing Our Partnership with Flowers Across
We are thrilled to announce our new collaboration with Flowers Across Sydney through their inspiring initiative, Givr...
Introducing Givr Charity by Flowers Across
Flowers Across Sydney is on a mission to make a difference with every bouquet they deliver. Through their Givr For...
Trekking for endo
By Tania Forlano I’ve supported Endometriosis Australia for a long time. As someone who was very familiar with effects...
Endometriosis Australia Go Sunny Solar Supporting Women’s Soccer in SA
As the mighty Matildas continue to kick goals ‘‘til it’s done’, Endometriosis Australia have joined with South...
From leaps to bounds: Workplace Accreditation Program, Research updates, and more!
I am pleased to bring you some exciting updates. Straight off the bat, I congratulate the Australian Women’s Cricket...
Brisbane High Tea
Endometriosis Australia’s Brisbane High Tea was fabulous, with keynote speakers Premier Annastacia Palaszczuk and...
Annastacia Palaszczuk Discusses Endometriosis on Today Show 9News
Queensland Premier Annastacia Palaszczuk discusses opening up about endometriosis on the Today Show after making an...
Study finds significant increase in endometriosis diagnoses and GP Referrals
Study Reveals Significant Increase in Endometriosis Diagnoses in Australian Women A new study has found the number of...
Pain clinic in your pocket: Australians living with endometriosis gain access to a game-changing platform
Endometriosis Australia partnered with CHARLI app to launch the first Australian hybrid technology and real-world...
Endometriosis in Australia is now estimated to be 1 in 7 females and those assigned female at birth
ENDOMETRIOSIS in AUSTRALIA AIHW Report 2023 1 in 7 females and those assigned female at birth, or 14% of girls and...
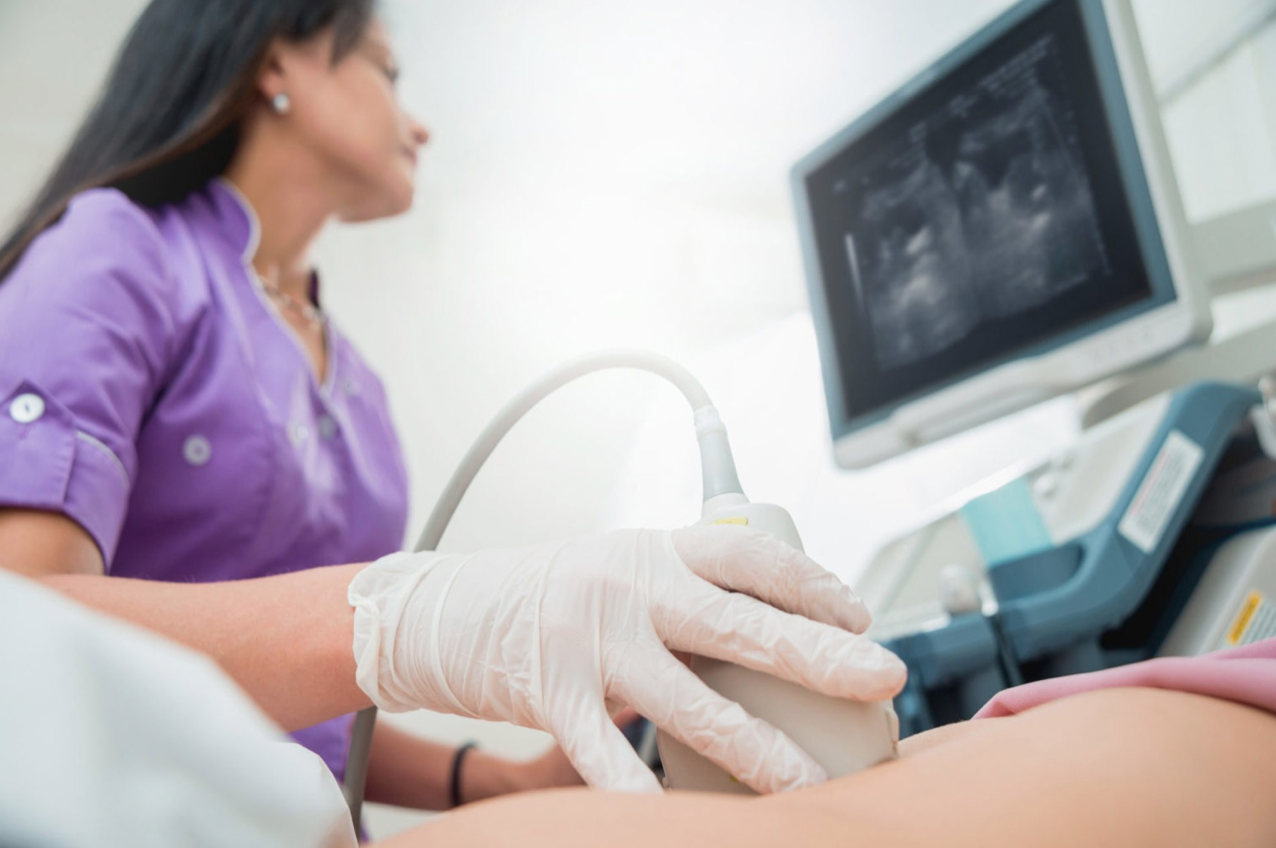
Can you be diagnosed with endometriosis from an ultrasound?
By Ms Alison Deslandes (IMAGENDO researcher) and A/Prof George Condous Endometriosis is a complex condition which can...
Pain science education for pelvic pain
What is pain science education? Pain science education aims to help people better understand what pain is, how it...
Genetics and endometriosis: What we know and how it can help treatment
Written by Dr Brett McKinnon, Research Fellow, Institute for Molecular Bioscience, UQ Endometriosis in the family It...
Why is it so difficult to get an endometriosis diagnosis?
In Australia, people with period pain or other gynaecological symptoms can wait on average of 6.4 years before their...
Inflammation and the menstrual cycle
What is the connection between inflammation and the menstrual cycle? This article breaks it down. What is the...
Anatomy 101 for surgical removal of endometriosis
Content warning: This article contains images that may be graphic for some readers. Knowing some basic knowledge of...
New Endometriosis Clinics in Australia
Locations for 11 new Endometriosis and Pelvic Pain Clinics announced The Federal Government has announced the...
Endometriosis Australia’s statement on Victorian Women’s Pain Inquiry
Women’s Pain Inquiry: A Turning Point for Endometriosis and Female Health Endometriosis Australia welcomes the...
EndoThrive Workplace Accreditation Program launches
EndoThrive Workplace Accreditation empowers businesses to build inclusive workplaces for nearly 1 million Australians...
Endometriosis Behind the Pain Panel
Endometriosis Australia’s Chair, Monica Forlano, joined a panel of leading gynaecologists, women’s health specialists,...
Podcast host Ellie Angel-Mobbs named finalist in Women In Media Awards
Endometriosis Australia’s podcast host recognised for championing change and breaking stigma in women's health We’re...
Endometriosis Australia welcomes $50 million commitment to research
20 May 2025MEDIA STATEMENT Endometriosis Australia welcomes $50 million commitment to research Endometriosis...
Endometriosis Research Funding and Contributions
7th April 2025MEDIA STATEMENT Endometriosis Australia Clarifies Research Funding and Contributions Endometriosis...
Tasmanian Government $1.2 million funding for endometriosis care 2025
31st March 2025MEDIA STATEMENT FOR IMMEDIATE RELEASE ENDOMETRIOSIS AUSTRALIA WELCOMES TASMANIAN GOVERNMENT'S $1.2...
Endometriosis Budget 2025 Australia: Boost for Women’s Health
MEDIA STATEMENT FOR IMMEDIATE RELEASE 26 MARCH 2025 Endometriosis Australia today welcomed the Federal Government's...
Endometriosis Truth and Awareness: Latest Podcast Episode
New Podcast Episode from The Briefing team: Addressing Marty Sheargold’s Harmful Comments on Endometriosis In light of...
7 ways to support someone with endometriosis
Endometriosis can be a difficult disease to manage, both for those who have it and those who love them and watch them...
Priority Populations in Endometriosis
Priority Populations in Endometriosis: Global and Cultural Perspectives Endometriosis affects an estimated 1 in 7...
Endometriosis and Pelvic Pain Clinics in Australia
Endometriosis and Pelvic Pain Clinics in Australia: Putting Patients First People living with endometriosis and...
Gender-Affirming Endometriosis Care
Gender-Affirming Endometriosis Care: Insights with Dr. Maddalena Giacomozzi Endometriosis is often described as a...
Age and Endometriosis with Dr Lydia Coxon
Age and Endometriosis: Understanding Flares Across the Lifespan Endometriosis is a chronic condition that affects...
Study finds significant increase in endometriosis diagnoses and GP Referrals
Study Reveals Significant Increase in Endometriosis Diagnoses in Australian Women A new study has found the number of...
Join the priority populations working group
Inclusive Endometriosis Education for Everyone in Australia Endometriosis Australia is proud to launch a new...
Endo-Friendly recipes by Alex Crisp!
Festive Season Show Stoppers by Alex Crisp, MasterChef and dedicated Endometriosis Australia Ambassador! Alex Crisp...
New scholarship for nurses to help Australians living with endometriosis
In collaboration with the Australian College of Nursing Foundation (ACNF), Endometriosis Australia is launching a new...
National Women’s Health Survey: Pelvic Pain in Australian Women 2023
Almost half (47%) of Australian women have experienced pelvic pain in the last five years, according to new research...
Transgender Awareness Week: Max Jahufer
Transgender Awareness Week: Max Jahufer on Endometriosis and Pelvic Pain Transgender Awareness Week is a time to...
Share your endometriosis story
Share Your Endometriosis Story Endometriosis Australia is calling for storytellers with lived experience of...
Adenomyosis Awareness Month
April is Adenomyosis Awareness Month. At Endometriosis Australia, we’re amplifying the voices of those affected by...
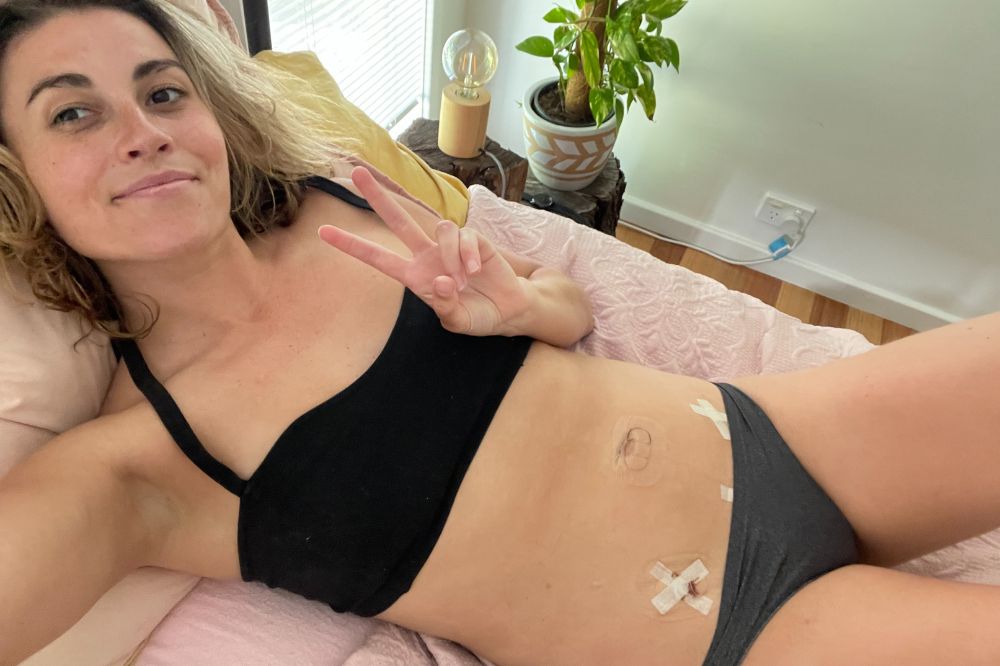
How I created a solution for thousands of endo warriors
Written by Kellie Johnson. The silence in the room was deafening. The technician applied more gel to my belly, pushing...
From Broken Bones to Breaking Barriers
Numerous broken bones, countless torn ligaments and dislocations, degenerating disks in my spine and bulging disks in...
Kendall Gilding Endometriosis Australia Ambassador opens up about her life living with endo
I've known endo from a young age. Watching my mum and older sister crippled in pain every month, with limited answers...
Trekking for endo
By Tania Forlano I’ve supported Endometriosis Australia for a long time. As someone who was very familiar with effects...
Turning Diagnosis into Determination
By Dr Eliza Colgrave I am an aggressive optimist, and my experience of living with endometriosis has played a big part...
The September 2023 edition of our national newsletter, brought to you amidst Jean Hailes’ Women’s Health Week
Wow, what an exciting, busy month it has been! Thank you for joining us for our September 2023 edition of our national...
EndoThrive Workplace Accreditation Program launches
EndoThrive Workplace Accreditation empowers businesses to build inclusive workplaces for nearly 1 million Australians...
Introducing Givr Charity by Flowers Across
Flowers Across Sydney is on a mission to make a difference with every bouquet they deliver. Through their Givr For...
From Broken Bones to Breaking Barriers
Numerous broken bones, countless torn ligaments and dislocations, degenerating disks in my spine and bulging disks in...
Endometriosis Australia launches first-ever national television campaign on endometriosis
Endometriosis Australia is launching its first television commercial (TVC) on July 15th, raising awareness about...
Kendall Gilding Endometriosis Australia Ambassador opens up about her life living with endo
I've known endo from a young age. Watching my mum and older sister crippled in pain every month, with limited answers...
Trekking for endo
By Tania Forlano I’ve supported Endometriosis Australia for a long time. As someone who was very familiar with effects...
Turning Diagnosis into Determination
By Dr Eliza Colgrave I am an aggressive optimist, and my experience of living with endometriosis has played a big part...
Endometriosis Australia Go Sunny Solar Supporting Women’s Soccer in SA
As the mighty Matildas continue to kick goals ‘‘til it’s done’, Endometriosis Australia have joined with South...
What to do if your friend has endometriosis
Have you got a BFF who’s recently confided in you that they’ve recently been diagnosed with endometriosis? If you...
Kayla Itsines’ endo story
Kayla Itsines tells her endo story. When I was 18, I found out that I have endometriosis. It’s an incredibly common...
Endo myth busting
I’ve been pretty consistently seeking out information about endometriosis since my diagnosis a few years ago. I’ve...
Pregnancy and endometriosis
For many women with endometriosis, the potential effect of the disease on their fertility is a concern. Reassuringly,...
H is for Hope
Over the past few years we have heard and seen much more discussion about the silent disease affecting individuals and...
Introducing Mackenzie Coonan: EndoChampion
Mackenzie Coonan is a journalist for 7 News in Brisbane, Queensland. Now twenty-seven, Mackenzie has been battling...
Introducing Fiona Stevens: EA Ambassador
Fiona is a lifelong Poet, Creative Collaborator, Wellbeing Australia Professional Member and Blue Mind Health...
Fertility preservation for women with endometriosis
Roger Hart CREI, Professor of Reproductive Medicine, University of Western Australia & Medical Director of...
A new look at endometriosis and infertility
By Dr Geoff Reid, Endometriosis Australia's Clinical Advisory Committee Endometriosis is estimated to affect over...
Surrogacy helped my dream come true
Prior to Australia’s annual surrogacy conference on 3-4 June, Sam Everingham looks at how one determined woman...
World Mental Health Day
Shining a Light on Endometriosis and Mental Health World Mental Health Day is a reminder that mental health is just as...
The October 2023 edition of our national newsletter
Welcome to the Endometriosis Australia Mental Health Month edition. We understand how endometriosis can affect your...
Jess Nathan – Finding Good Care in Remote Australia
I was in my early 20’s when I was first diagnosed with endometriosis. After years of painful and debilitating periods...
Healing body image with endometriosis
Having endometriosis can have a profound impact on our relationship with our body. Many people that have challenging...
Why calming down the nervous system can help endometriosis
Endometriosis-related pain levels are not always related to the extent of endometrial lesions. For many people, pain...
7 ways to support someone with endometriosis
Endometriosis can be a difficult disease to manage, both for those who have it and those who love them and watch them...
Endometriosis and quality of life
We know that endometriosis is a chronic disease that can lead to symptoms such as period and/or pelvic pain, fatigue,...
The pain of endo
A couple of weeks ago I participated in an online survey as part of Macquarie University’s research project titled The...
200 million people have endo
A couple of weeks ago I had one of the most brutal periods I’ve ever experienced. The pain, coupled with bouts of...
It takes a village
Endo can be a lonely disease. There are times, particularly during my period, where I feel as if I’m the only one...
Endometriosis and relationships
By Ash As I sit here looking at my engagement ring, I realise that there is still hope. I have been fighting...
EndoThrive Workplace Accreditation Program launches
EndoThrive Workplace Accreditation empowers businesses to build inclusive workplaces for nearly 1 million Australians...
Supporting endometriosis at work
For around one in seven Australian women and those presumed female at birth, going to work can mean pushing through...
About Us
Endometriosis Australia is a nationally accredited charity that endeavours to increase recognition of endometriosis, provides endometriosis education programs, and provides funding for endometriosis research.