Endometriosis is a complex condition which can be challenging to diagnose. Historically, diagnosis relied upon key-hole surgery (called laparoscopy). However, advances in imaging technology means that international guidelines now recommend an endometriosis ultrasound. This means an ultrasound can be used in the diagnostic work-up of endometriosis and, in some cases, can replace the need for laparoscopy for diagnosis.
The different types of endometriosis
Endometriosis is characterised by tissue which is similar to the lining of the uterus depositing outside of the uterus in little spots called lesions. Endometriosis lesions are categorised in different ways depending on in their size, location, and appearance. The three most common types of endometriosis are superficial endometriosis, ovarian endometriosis and deep endometriosis.
- Superficial endometriosis are tiny lesions over the surface of organs in the pelvic region and in the layer of tissue which lines the pelvic and abdominal cavities (called the peritoneum). They are typically only a few millimetres wide and deep (imagine pimples but on the inside of the body).
- Ovarian endometriosis occurs when endometriosis grows in the ovary, causing an ovarian cyst called an endometrioma.
- Deep endometriosis can grow throughout the pelvis. It may be found in the bladder, bowel, back of the cervix and uterosacral ligaments (the ligaments which suspend the uterus to the back of the pelvis) and sometimes in other locations beyond the pelvis.
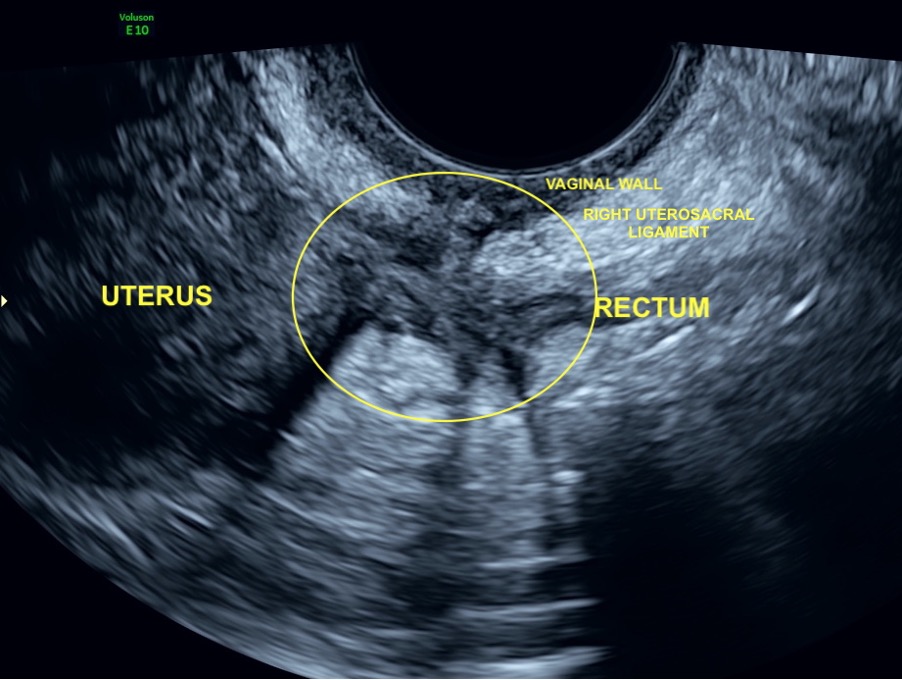
A transvaginal ultrasound image showing a nodule of deep endometriosis. The area circled in yellow is a nodule of deep endometriosis within the right uterosacral ligament. It is stuck to the adjacent vaginal wall, rectum and uterus and causing distortion to these anatomical areas.
Endometriosis often occurs along with a condition called adenomyosis, in which endometrial tissue deposits into the muscle of the uterus, causing heavy bleeding and pain.
What is an ultrasound?
Ultrasound uses high-frequency sound waves to view the internal organs. To look for endometriosis in the pelvis, a type of ultrasound called a transvaginal ultrasound is used. This is performed by a sonographer or sonologist inserting a slender camera into a person’s vagina to obtain the images. Some people can find a transvaginal ultrasound uncomfortable (especially if they are experiencing pelvic pain at the time of the scan), but in most cases it is well tolerated even in young people or those that aren’t sexually active. Ultrasound scans are safe and widely available, which is why they are the go-to imaging tool used by gynaecological specialists.
How does ultrasound detect endometriosis?
To look for endometriosis on ultrasound, the sonographer or sonologist performing the scan will systematically assess the areas of the pelvis known to commonly be affected by endometriosis.
Typically, the scan will start by assessing the uterus and the ovaries for adenomyosis and ovarian endometriomas (endometriosis cysts).
Next, they will try to move the organs by applying some pressure internally with the camera or externally with their hand. This shows whether there may be adhesions present, or a condition called ‘obliteration of the pouch of Douglas’ in which the bowel sticks to the back of the uterus.
The final aspect of the scan will be to carefully assess the areas in front of and behind the uterus (called the anterior and posterior pelvic compartments) to detect nodules of endometriosis in locations such as the rectum, uterosacral ligaments, vaginal walls, bladder and ureters. If endometriosis is present, this will typically look like dark spots in these locations which can range in size from a few millimetres to several centimetres. If adhesions are present, the organs will move together rather than away from each other when pressure is applied. Research has shown that when performed in this way, ultrasound has a high level of diagnostic accuracy for endometriosis, especially for moderate or severe disease.
I’ve had multiple ultrasounds which have been normal, but at surgery I had endometriosis everywhere. Why were my scans normal?
Unfortunately, this is a common occurrence and exceedingly frustrating for those suffering with endometriosis symptoms. This can occur for a few reasons.
The most common reason for endometriosis (even severe disease) not being detected by ultrasound is that it wasn’t looked for. The standard pelvic ultrasound typically performed in Australia will only assess the uterus and ovaries meaning any disease in front of, or behind the uterus will not be seen. As endometriosis most commonly occurs behind the uterus (in the posterior compartment), this is a common reason for disease being “missed” on ultrasound. To maximise the chances of endometriosis being detected by ultrasound, booking in to have scans in clinics which specifically offer “endometriosis ultrasound” or those specialising in gynaecological imaging is recommended. At this stage however, there is no clear accreditation or credentials in Australia for imaging practices which easily identify them as experts in endometriosis imaging.
Additionally, as the techniques to detect endometriosis with ultrasound are still new, imaging professionals across the country are having to learn different skills which takes time. In very heartening news for those suffering from endometriosis, Australian sonographers are embracing this learning extremely well and it is likely quality of scanning and access to good quality scans with sonographers who are skilled in detecting endometriosis will improve significantly in the coming years.
So, is an endometriosis ultrasound foolproof?
Scans can be normal in people who have only superficial deposits of endometriosis. Due to the very small size of these lesions, an ultrasound, even when performed by someone very experience in endometriosis detection, won’t always find these lesions, although a lot of research is occurring to try and change this. Because of this, it is essential to know that if the scan is normal, this does not exclude endometriosis and if symptoms are problematic, discussion with your doctor about further diagnostic investigation is essential.
If you are experiencing endometriosis symptoms, it’s important to speak to your GP, gynaecologist, or an endometriosis specialist to get a diagnosis. These doctors can all refer for an endometriosis ultrasound as part of the diagnostic work-up. The sooner you get a diagnosis, the sooner you can get treatment.
Imaging is a key part of the diagnosis of endometriosis. Not only can imaging provide an answer as to why you’ve been experiencing horrible symptoms, it can open to door appropriate treatment which can minimise potential complications and improve quality of life.
Ms Alison Deslandes is a specialist obstetric and gynaecological sonographer and endometriosis researcher with the IMAGENDO group at the University of Adelaide.
A/Prof George Condous is an expert gynaecological sonologist and specialist endometriosis laparoscopic surgeon. He is a world-leading researcher on the topic of ultrasound for the diagnosis of endometriosis.